What Is Rectal Bleeding?
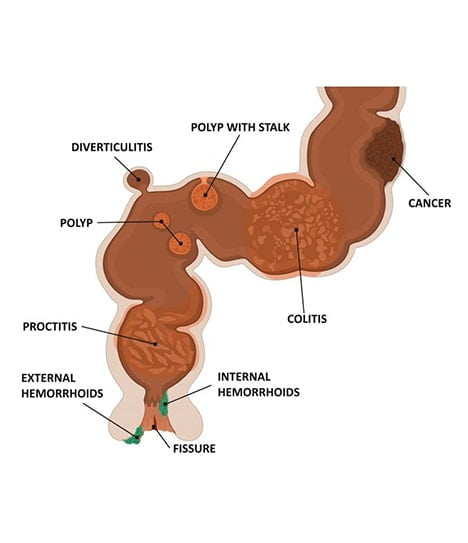
Rectal bleeding (medically known as hematochezia) refers to any blood passing from your anus. However, rectal or anal bleeding is commonly assumed to refer to bleeding from the rectum or your colon. It can manifest as blood in your stool, toilet paper, or the toilet bowl. The blood in the stool caused by anus bleeding from the anus can range from bright red to dark maroon to a dark tarry color.
Rectal bleeding can be a symptom of colorectal or anal cancer, which can be treated if caught early. In addition to a complete physical exam and medical history, colonoscopy is the gold standard for visual evaluation of your colon for an accurate diagnosis. It can detect polyps, mass lesions, abnormalities of the intestine lining, and a variety of other causes of your symptoms.
This condition can also be caused by bleeding hemorrhoids, anal fissures, colitis, or other diagnosable and treatable conditions. Disorders higher up in the digestive tract can also lead to bleeding from the anus.
For these reasons, consulting an experienced gastroenterologist is the first step in determining the underlying causes of rectal bleeding and the best hematochezia treatment options. To perform the proper treatment, we must first correctly diagnose the cause. Internal hemorrhoids and anal fissures are two common causes of anal bleeding. Colonoscopy, in combination with a thorough physical exam, is the gold standard for visual evaluation of the colon for diagnosis. We can treat these diseases more effectively if we diagnose, detect, and address them early.
”
★ ★ ★ ★ ★The entire staff was welcoming and made the visit quick and seamless. The office is clean, and the staff even make a point in offering coffee or water while you wait. The doctor was very friendly and to the point. Highly recommend choosing this office.
According to the study “Factors identifying higher risk rectal bleeding in general practice” published on PubMed: “Rectal bleeding is common in the community and may be an early symptom of bowel cancer. The most useful factors in identifying higher risk groups were anus bleeding in combination with a change in bowel habit to looser stools and/or an increased frequency of defaecation, bleeding without perianal symptoms, and age over 60 years.”
Read more: Anal Cancer: Are You at Risk?
What Are the Symptoms of Rectal Bleeding?
Rectal bleeding symptoms include:
- Straining and constipation
- Abdominal pain
- Itching
- Swelling around the anus
- Skin problems
- Bloody diarrhea
What Causes Rectal Bleeding?
Rectal bleeding can occur for a variety of reasons, ranging from harmless gastrointestinal tract conditions such as bleeding hemorrhoids and anal fissures to more serious conditions such as cancer.
Rectal bleeding causes include:
- Hemorrhoids
- Anal Fissures
- Anal Cancer
- Colon Cancer
- Ulcerative Colitis/Crohn’s Disease
- Solitary Rectal Ulcer (ulcer in the rectum)
- Diverticulosis (a bulging pouch)
- Proctitis (inflammation of the rectum)
- Ischemic colitis (a colon inflammation)
- Infectious Colitis (inflammation of the colon)
Colon Cancer
Colorectal and anal cancers are more serious causes of rectal bleeding. Colon cancer, the second leading cause of cancer deaths in the United States, begins in the large intestine. Because it is a slow-growing disease, early detection allows us to effectively treat it. Most cases of colon cancer come from polyps in your colon. Finding and removing polyps through a colonoscopy reduces your cancer risk. Anal cancer is less common but also curable when diagnosed early.
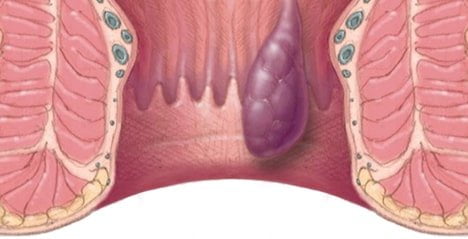
Hemorrhoids
Hemorrhoids are inflamed or swollen veins just below the surface of the skin. They can occur around your anus (external hemorrhoids) or inside your anal canal (internal hemorrhoids). Already sensitive, they can easily cause bleeding from the rectum if irritated.
Common causes of hemorrhoids are:
- Sitting on the toilet too long
- Straining during bowel movements
- Aging
- Chronic diarrhea or constipation
- Pregnancy
- Obesity
- A low-fiber diet
The condition usually is signaled by itching, discomfort, and bleeding from the rectum. If blood pools in an external hemorrhoid, it may form a clot called a thrombosed external hemorrhoid.
Anal Fissures
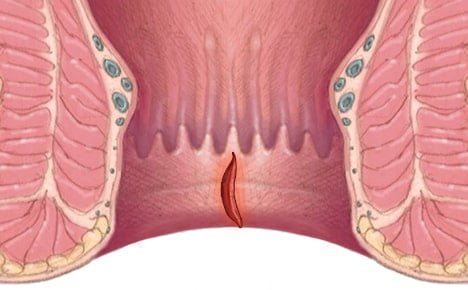
Anal fissures are tears in the lining of your anus. They usually appear after bouts of constipation, hard stools, diarrhea, or inflammation. Anal fissures can cause pain during and immediately after a bowel movement and bleeding from the anus. You may also experience spasms in the ring of muscle at the end of your anus.
Proctitis
Proctitis is a medical condition that occurs when the lining of your rectum and the rectal lining become inflamed, potentially leading to pain. The symptom of proctitis can include anus bleeding.
Causes of proctitis include:
- An infection
- Certain medications
- Prior radiation therapy for cancer treatment
- Some forms of inflammatory bowel disease (IBD)
Diagnosing Anal Bleeding
They may:
- Feel for abnormalities within your rectum with a gloved, lubricated finger
- Examine your anus visually and using an anoscope during the physical exam
- Perform a colonoscopy for direct visualization of your colon, which is the gold standard for evaluation
How is Rectal Bleeding Treated?
Anal bleeding treatment depends on the underlying cause. Most cases of anal fissures, hemorrhoids, or constipation can be managed with simple dietary adjustments to improve bowel habits. Boosting fiber consumption, staying hydrated, and taking certain medications are common options prescribed by the best rectal bleeding specialist in NYC. Warm baths can also help relieve discomfort from hemorrhoids or anal fissures.
If the cause of the condition is bleeding hemorrhoids, our doctors may recommend infrared coagulation (IRC), hemorrhoid banding, or other cutting-edge treatments as the definitive response to stubborn hemorrhoids. For large or persistent hemorrhoids that don’t respond to treatment, surgical removal may be necessary. These approaches are part of our comprehensive rectal bleeding treatment in NYC, tailored to your specific needs.
For more serious cases, such as rectal bleeding caused by colon cancer or diseases like ulcerative colitis, surgery might be required. If colon or anal cancer is the cause, chemotherapy or radiation therapy may also be part of the treatment plan.
When Should You Worry About Rectal Bleeding?
Bleeding from the anal area should always be evaluated by a gastroenterologist for an accurate diagnosis and blood in the stool treatment plan, since it may be a symptom or sign of a serious illness or condition.
When should you see a doctor for rectal bleeding? You should seek immediate emergency help if you have significant bleeding from the rectum and any of the following symptoms:
- Rapid and shallow breathing
- Blurred vision
- Dizziness after standing up
- Fainting
- Nausea
- Confusion
- Cold and pale skin
- Low urine output
- Heavy rectal bleeding
- Accompanied by severe abdominal cramping or pain
Frequently Asked Questions
Can Medications Cause Bleeding From Anus?
GI bleeding may result from the use of oral anticoagulants. Hemorrhoidal bleeding can also be associated with medications that lead to constipation. Other triggers and drugs that cause rectal bleeding could be advancing age, the use of multiple medications, drug-drug interactions, and health-related disorders.
Are There Any Home Remedies for Rectal Bleeding?
Bleeding rectum treatment depends on the root cause of the problem. Several natural remedies can help you address bleeding from the anus.
These natural remedies are:
- Relieve constipation
- Calm bleeding hemorrhoids
- Improve ulcerative colitis
- Soften stools
- Reduce your stress level
Even though the recommendations mentioned above are considered helpful, you should talk to your healthcare provider before starting treatment.
Can Stress Cause Bleeding Out of Rectum?
Stress does not typically lead to ulcerative colitis. However, chronic stress can harm your immune system and trigger chronic inflammation. It will increase ulceration and cause bleeding. While it is impossible to eliminate all stress, you can learn how to handle your emotions and stress. Try to avoid the consumption of caffeine and alcohol, which can stimulate intestinal contractions and worsen diarrhea. Caffeine and alcohol might also worsen stress and anxiety.
Is Bright Red Blood in the Stool Worse than Darker Blood?
Are There Any Foods That Can Cause Red or Black Stools?
Consumption of certain foods can lead to red or black stools.
Foods that can cause red-colored stools include:
- Beets
- Tomato juice or soup
- Cranberries
- Red licorice
- Food that is dyed red
Foods that can result in unusually dark stools include:
- Black licorice
- Blueberries
- Dark leafy vegetables
- Blood sausage
In addition, certain iron pills or bismuth-containing medications (such as bismuth subsalicylate or Pepto-Bismol) can also change the color of your stool to black or other colors.
Will Rectal Bleeding Go Away on Its Own?
Important Reminder: The only intent of this information is to provide guidance, not definitive medical advice. Please consult a doctor about your specific condition. Only trained, experienced physicians like our specialists can determine an accurate diagnosis and proper rectal bleeding treatment.
When experiencing bloody bowel movements, consult a rectal bleeding specialist to determine the cause and receive appropriate care. The expert team at Manhattan Gastroenterology uses advanced tools to diagnose and treat your condition effectively. Our best-in-class gastroenterologists have earned esteemed reputations for providing personalized, comprehensive care. For more info about your rectal bleeding treatment options in the Upper East Side or Midtown NYC or to schedule an appointment with one of our rectal bleeding doctors, please contact our offices.



















