Hemorrhoid Treatment Specialists
Our board-certified gastroenterologists specialize in minimally invasive hemorrhoid treatments. We offer in-office, non-surgical removal of hemorrhoids using infrared coagulation (IRC) and hemorrhoid banding for swollen and inflamed veins in the anus or lower rectum. Our doctors have received specialized training in the use of IRC and have successfully treated a large number of patients suffering from internal hemorrhoids.
 ★★★★★
Dr. Divya Mallam
Gastroenterologist
★★★★★
Dr. Divya Mallam
Gastroenterologist
 ★★★★★
Dr. Dana Zhao, MD
Gastroenterologist
★★★★★
Dr. Dana Zhao, MD
Gastroenterologist
 ★★★★★
Dr. Michael Rosman, MD
Gastroenterologist
★★★★★
Dr. Michael Rosman, MD
Gastroenterologist
 ★★★★★
Dr. Michael Schopis, MD
Gastroenterologist
★★★★★
Dr. Michael Schopis, MD
Gastroenterologist
 ★★★★★
Dr. Connie Park, MD
Gastroenterologist
★★★★★
Dr. Connie Park, MD
Gastroenterologist
 ★★★★★
Dr. Qin Rao, MD
Gastroenterologist
★★★★★
Dr. Qin Rao, MD
Gastroenterologist
 ★★★★★
Dr. Daniel Perl, MD
Gastroenterologist
★★★★★
Dr. Daniel Perl, MD
Gastroenterologist
 ★★★★★
Lauren Schwartz, MD
Gastroenterologist
★★★★★
Lauren Schwartz, MD
Gastroenterologist
 ★★★★★
Eric Yoon, MD
Gastroenterologist
★★★★★
Eric Yoon, MD
Gastroenterologist
 ★★★★★
Kristen Lee, MD
Gastroenterologist
★★★★★
Kristen Lee, MD
Gastroenterologist
 ★★★★★
Mikhail Yakubov, MD
Gastroenterologist
★★★★★
Mikhail Yakubov, MD
Gastroenterologist
 ★★★★★
Michael Dann, MD
Gastroenterologist
★★★★★
Michael Dann, MD
Gastroenterologist
 ★★★★★
Shawn Khodadadian, MD
Gastroenterologist
★★★★★
Shawn Khodadadian, MD
Gastroenterologist
 ★★★★★
Aga Nagorna, MD
Gastroenterologist
★★★★★
Aga Nagorna, MD
Gastroenterologist
 ★★★★★
Kathryn Schmidt, MD
Gastroenterologist
★★★★★
Kathryn Schmidt, MD
Gastroenterologist
 ★★★★★
Julia Boroday, AGNP-C
Gastroenterologist
★★★★★
Julia Boroday, AGNP-C
Gastroenterologist
Our doctors, top-rated NYC gastroenterologists, and hemorrhoids specialists at Manhattan Gastroenterology offer a variety of hemorrhoids treatments based on the severity of the condition. Topical medications and a healthier diet can alleviate the symptoms in mild cases. In other cases, laser hemorrhoid treatment, IRC (Infrared Coagulation), hemorrhoid banding, or, rarely, surgery to physically remove the hemorrhoids can be performed.
What Are Hemorrhoids?
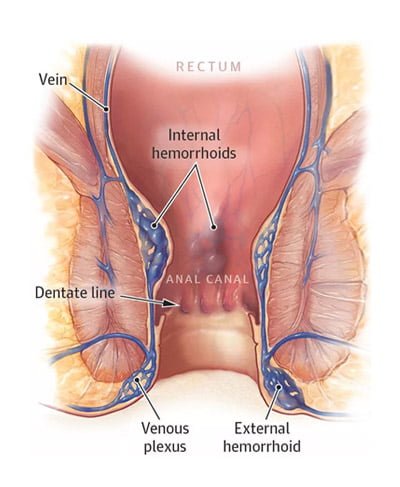
Hemorrhoids are swollen and inflamed veins that can cause discomfort and bleeding in the rectum and anus. If you suspect hemorrhoidal disease, you should always be evaluated with a thorough consultation and examination by a physician for an accurate diagnosis, treatment plan and to exclude a serious illness or condition such as colon or anal cancer. Hemorrhoidal disease is just one of the many causes of rectal bleeding and lesions around the anus that need evaluation. Rectal bleeding can be a symptom of any type of colorectal or anal cancer, which can be cured if detected early.
Piles are extremely common. Piles are a very common occurrence. Approximately half of the population develops symptoms of this health condition by the age of 50 [1]. Internal hemorrhoids form inside your anal canal, whereas external hemorrhoids form under the skin around your anus. If blood pools in an external hemorrhoid, it may form a clot called a thrombus. This condition can result in severe pain and inflammation.
This health condition can be very painful. For the best hemorrhoid treatment options, including laser hemorrhoid treatments, see our NYC hemorrhoids doctors. Emergency appointments are available at the NYC doctor’s office.
Infrared coagulation and hemorrhoid banding are two minimally invasive and effective treatment options offered by our trained and rated hemorrhoid doctors.
What Are the Treatments We Offer at Manhattan Gastroenterology?
Our doctors at Manhattan Gastroenterology are not only top-rated NYC gastroenterologists. They’re also top-of-the-line hemorrhoid specialists. They offer a variety of hemorrhoidal disease treatments, including minimally invasive laser hemorrhoid treatments and other effective options.
In mild cases, topical medications and conservative treatment such as sitz baths and laxatives can help to alleviate symptoms. In other cases, we can perform IRC (Infrared Coagulation), hemorrhoid banding, or rarely surgery to remove the piles. A complete evaluation and diagnosis by your hemorrhoid doctor are very important for an accurate diagnosis and treatment plan.
When Should I See My Hemorrhoid Doctor?
You should see a hemorrhoid specialist if you feel discomfort and pain in the rectum, especially when you sit or notice blood when wiping. Don’t put off seeing a doctor if you notice your hemorrhoids bleeding, symptoms get drastically worse or if they start interfering with your daily activities. Seek emergency medical care immediately if you experience a large amount of rectal bleeding (including painless bleeding) accompanied by dizziness.
If you observe blood when wiping or have discomfort and pain in your rectum, especially when you sit, you should see a hemorrhoid specialist. If your hemorrhoids start bleeding, your symptoms worsen, or they start interfering with your daily activities, visit a doctor right away. If you have a large amount of rectal bleeding (including painless bleeding) and dizziness, get emergency medical care immediately.
Hemorrhoid Doctor Near Me: Get Expert Diagnosis & Lasting Relief at Manhattan Gastroenterology
Whether dealing with internal or external hemorrhoids, choose a team of board-certified gastroenterologists specializing in the diagnosis and management of the most common anorectal diseases, ranging from topical and medical therapies to outpatient treatments and surgical interventions.
How To Find the Best Hemorrhoids Clinic Near You
Consider using the following guidelines for finding a medical professional in your area:
- Ask your friends or relatives for recommendations.
- Search online using phrases like “hemorrhoid doctors near me,” “hemorrhoid specialist near me,” or “hemorrhoid treatment near me.”
- Check online reviews of nearby hemorrhoid specialists.
- Discuss your treatment options with a couple of specialists by scheduling an appointment.
Leading hemorrhoid doctors at Manhattan Gastroenterology offer expert diagnosis and a range of personalized non-operative and operative treatments for hemorrhoids. Tailored to individual preferences, convenience, and the severity of hemorrhoids, our expert approach ensures enduring relief from issues such as rectal bleeding, prolapse, and pruritus.
For mild cases, symptom alleviation can be achieved through topical medications and adopting a healthier diet. In more advanced cases, cutting-edge treatments such as laser hemorrhoid treatment, IRC (Infrared Coagulation), hemorrhoid banding, or, in rare instances, surgical removal of hemorrhoids may be recommended to address the condition effectively.
What Are the Symptoms of Hemorrhoids?
Hemorrhoids have different symptoms and signs depending on the type, but the most common symptom is rectal bleeding when passing stools. Blood does not usually mix with the stool, but instead coats the outer surface or is visible on toilet paper. The blood is usually a bright red color and may be visible in the toilet.
Rectal bleeding, however, should always be evaluated by a physician or your local hemorrhoids treatment doctor, as it can be a symptom of a severe underlying condition, such as cancer.
Other hemorrhoid symptoms include:
- Itching around the anus
- Blood on your tissue after having a bowel movement
- An itchy or painful lump or swelling near your anus
- Painful bowel movements, irritation, and pain around the anus
- Rectum pain while sitting and many other signs
What Are the Causes of Hemorrhoids?
Hemorrhoids can be caused by a variety of factors, but the exact cause is often unknown. Traditionally, this health issue has been linked to constipation or straining during bowel movements. When people have to sit on the toilet for an extended period of time, it might obstruct blood flow to and from the area. Sitting on the toilet for a long time can cause blood to pool, enlarging the blood vessels.
Hemorrhoids can form inside your anal canal (internal hemorrhoids) or under the skin around your anus (external hemorrhoids).
How To Classify and Diagnose Hemorrhoids?
As part of your evaluation, our gastroenterologists will perform a thorough physical examination, including a rectal exam and anoscopy, in our NYC offices. An anoscopy is a procedure in which a light-emitting device called an anoscope is gently inserted into the anus, allowing your physician to better visualize the tissues in your anorectal area.
Our GI hemorrhoids doctors may also suggest a colonoscopy for seeing your colon in detail and to rule out other, more serious causes of your symptoms. Colonoscopy is the gold standard for visualizing the whole colon in order to make an accurate diagnosis.[2]
There are three types of hemorrhoids:
- internal hemorrhoids (above the dentate line)
- external hemorrhoids (below the dentate line)
- mixed hemorrhoids (above and below the dentate line)
The specialist may suggest colonoscopy for full visualization of your colon and to rule out other more serious causes of your symptoms.
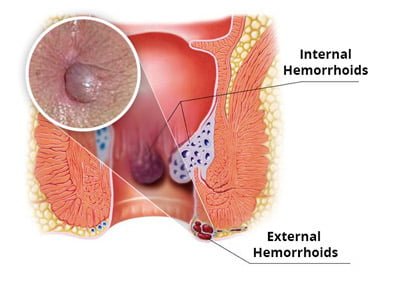
Internal Hemorrhoids
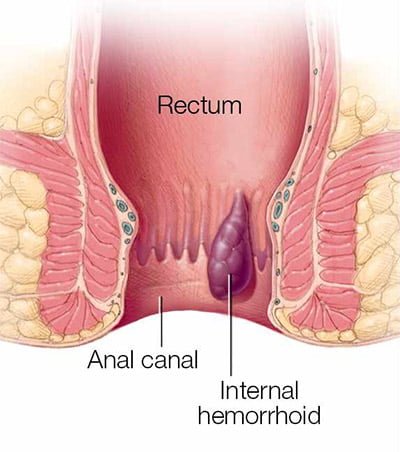 Internal hemorrhoids are located within the rectum and are not frequently felt or visible. You may bleed when passing a stool if you have the internal hemorrhoidal disease. Hemorrhoids can push through the anal opening as a result of straining, causing irritation and pain when they prolapse or protrude. When the veins in your lower rectum or anus swell and bulge outward, you get a prolapsed hemorrhoid.
Internal hemorrhoids are located within the rectum and are not frequently felt or visible. You may bleed when passing a stool if you have the internal hemorrhoidal disease. Hemorrhoids can push through the anal opening as a result of straining, causing irritation and pain when they prolapse or protrude. When the veins in your lower rectum or anus swell and bulge outward, you get a prolapsed hemorrhoid.
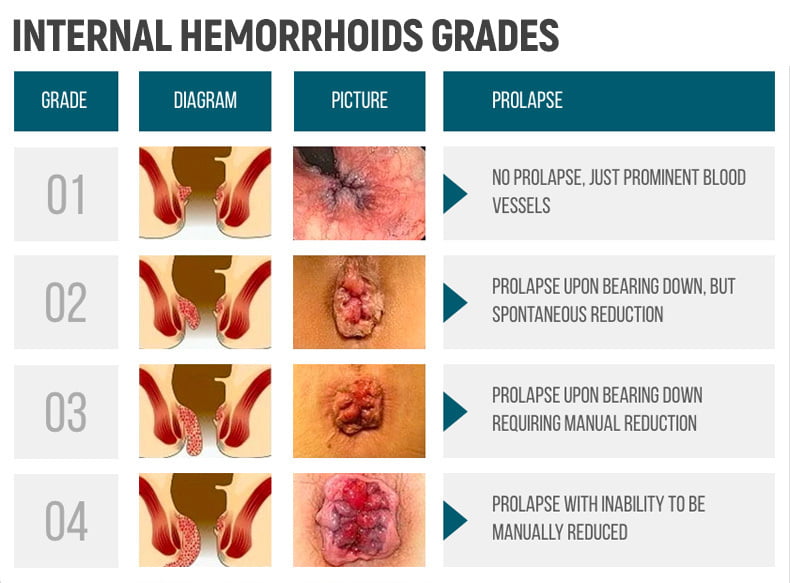
Internal hemorrhoids are categorized and treated differently depending on the degree of prolapse:
- Grade I: These are non-prolapsing hemorrhoids.
- Grade II: These are piles that prolapse on straining but which reduce naturally.
- Grade III: These are prolapsing hemorrhoids that require manual reduction.
- Grade IV: These are prolapsing, non-reducible hemorrhoids, including incarcerated hemorrhoids and acutely thrombosed hemorrhoids (incarcerated hemorrhoids are prolapsed hemorrhoids that we cannot reduce into the anal canal).
However, if internal hemorrhoid bleeding is causing you pain and discomfort, you should get medical assistance from the best hemorrhoid doctors in NYC. A physician should always evaluate your symptoms to ensure an accurate diagnosis and treatment plan and rule out serious illnesses or conditions such as colon or anal cancer.
External Hemorrhoids
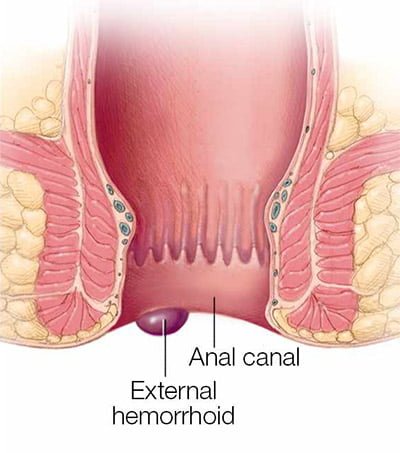 These are piles that develop beneath the skin surrounding the anus and can become thrombosed. You may notice signs and symptoms such as pain and bleeding. The area around your anus may be swollen. You may also have irritation or itching in the anal region. We recommend conservative therapies if external hemorrhoids become acutely thrombosed. A colorectal surgeon may refer you for excision in certain cases.
These are piles that develop beneath the skin surrounding the anus and can become thrombosed. You may notice signs and symptoms such as pain and bleeding. The area around your anus may be swollen. You may also have irritation or itching in the anal region. We recommend conservative therapies if external hemorrhoids become acutely thrombosed. A colorectal surgeon may refer you for excision in certain cases.
Prolapsed Hemorrhoids
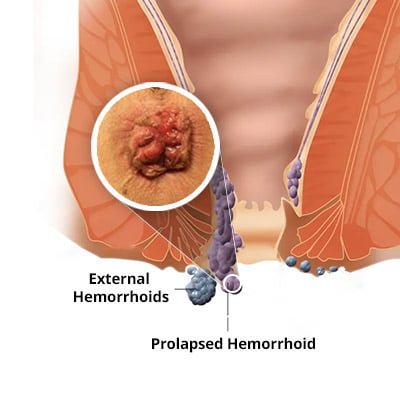
A prolapsed hemorrhoid occurs when a vein in your lower rectum or anus swells and creates hemorrhoids, resulting in an outward bulge. A prolapsed hemorrhoid can be very painful. The main symptom of a prolapsed hemorrhoid is the sensation of one or more lumps around the anus. However, this usually happens only if there is a significant prolapse.
It may be possible to gently push the lump back into the anus, but this merely changes the piles’ location and will not fix the problem. Prolapsed hemorrhoids tend to be quite painful when sitting and can hurt during bowel movements.
Protrusive hemorrhoids can collect small amounts of tiny stool particles and mucus, potentially causing an irritation called pruritus ani. Unfortunately, continually wiping the area to relieve the itching can worsen the irritation.
What Causes a Prolapsed Hemorrhoid?
Hemorrhoids can prolapse when the connective tissues that hold them in place weaken. One possible reason is straining during bowel movements, which is especially likely if you have diarrhea or constipation.
Pregnancy also raises the risk, with up to 40% of pregnant women having hemorrhoids that can prolapse if left untreated. Another risk factor is obesity, which puts extra strain on the rectal veins, increasing the likelihood of piles and prolapsed internal and external hemorrhoids. Cigarette smoking can damage your blood vessels, including those in your anus and rectum, increasing your risk of hemorrhoidal disease and prolapsed hemorrhoids.
Thrombosed Hemorrhoids
If a blood clot or thrombus has formed within the prolapsed hemorrhoid, it can be extremely painful. This is referred to as a thrombosed hemorrhoid. A thrombosed hemorrhoid can become acute and is more common in those who have severe constipation or a history of straining for long periods.
The pain is usually the worst within the first 24 to 48 hours. After this period has passed, the thrombus is gradually absorbed, reducing pain. A thrombosed hemorrhoid can look like a blue-colored lump.
Although a thrombosed hemorrhoid isn’t as dangerous as developing blood clots in other areas of the body, you may require professional help to drain it and relieve severe pain. Prolapsed hemorrhoids can also be painful if they become strangulated, which occurs when the blood supply to the hemorrhoid is cut off.
Symptoms of a thrombosed hemorrhoid include:
- Swelling
- A hard lump near the anus
- Inflammation
- Pain which may be severe
Pregnancy Hemorrhoids
Excisional haemorrhoidectomy is a surgical technique used to remove the excess tissue that is causing the bleeding. The surgery can be carried out under general anesthesia, spinal anesthesia, or sedation. It is a highly effective treatment for severe and recurring hemorrhoids, and it cures 95 % of cases. The risk of complications is low. During surgery, one or more incisions are made near hemorrhoid to remove it. The incisions are then either closed or left open.
Hemorrhoid Treatment Options
Our doctors at Manhattan Gastroenterology are top-rated New York City gastroenterologists and hemorrhoid specialists that offer varied hemorrhoidal disease treatments based on severity. In mild cases, conservative therapy may include sitz baths, laxatives, over-the-counter (OTC) or prescription medications. In other cases, we can remove the piles via IRC (Infrared Coagulation), hemorrhoid banding, or, in rare cases, surgery. A thorough evaluation and early diagnosis by your top hemorrhoid doctor specialist are necessary for an accurate diagnosis and treatment plan.
Our renowned Manhattan gastroenterologists are among the best in the field, specializing in the treatment and prevention of conditions related to swollen and inflamed veins in the rectum, referred to as hemorrhoids. You may finally put an end to your search for a “hemorrhoid specialist near me” and call the best-rated team of gastroenterologists, leading hemorrhoidal disease treatment doctors in NYC for an appointment. A board-certified “hemorrhoid doctor near me” specialist who will not only help you with your pain but also employs the latest cutting-edge hemorrhoidal disease treatments. Our gastroenterologists in New York might recommend one of the minimally invasive nonsurgical procedures, including hemorrhoid banding and IRC (Infrared Coagulation).
For more information about the best bleeding hemorrhoid NYC treatment or to schedule a consultation with one of our hemorrhoids specialist GI doctors, please contact our office.
Laser Treatment for Hemorrhoids
While there are other methods for treating hemorrhoids, laser hemorrhoid removal is the most effective, fast-acting, and best hemorrhoid treatment option. Our doctors, who are best-in-class Upper East Side NYC gastroenterologists, have undergone special training in using IRC and have successfully treated many patients.
Laser hemorrhoids treatment uses infrared light, a laser, or an electrical current with the same efficiency. We conduct infrared coagulation on an outpatient basis in the doctor’s office. We may administer mild sedation as necessary for the hemorrhoid laser surgery procedure, which usually only takes a few minutes.
The use of a laser for hemorrhoids has been shown to improve bleeding and pain in patients with internal and external hemorrhoids.
The laser hemorrhoid treatment procedure has been shown to be more effective than rubber band ligation in reducing postoperative pain, resolving symptoms, and improving quality of life in patients with grade II or III hemorrhoids with incomplete mucosal prolapse.
What Is Infrared Coagulation?
Infrared coagulation is a minimally invasive, cutting-edge office-based treatment option that uses infrared light or heat to treat hemorrhoidal disease. Infrared Coagulation (IRC) has quickly become one of the most popular office laser hemorrhoid treatments.
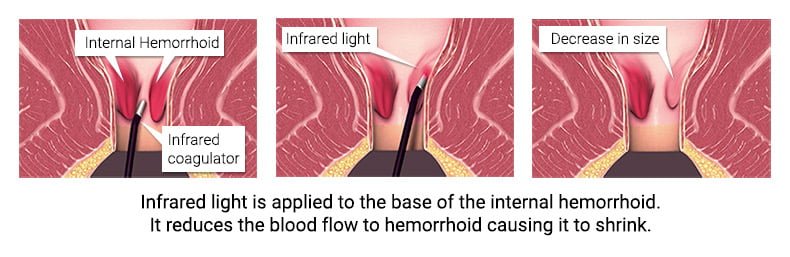
The IRC, or infrared coagulator, contains a light source at its tip that applies heat to the hemorrhoid column’s base. This procedure causes scar tissue to form at the site, which can result in the hemorrhoid column diminishing or disappearing. This procedure is usually well tolerated with minimal side effects. Each treatment will only take a few minutes, and you may need several treatments to cover all areas. Patients are often able to return to work and other regular activities shortly following the treatment.
Why You May Need Infrared Coagulation?
Infrared coagulation is effective in treating both small and medium-sized hemorrhoids. If you have irritating internal hemorrhoids that continue to cause pain, bleeding, and other symptoms despite conservative treatment, IRC treatment for hemorrhoids in NYC may be the answer.
What Happens During the IRC Procedure?
During the infrared coagulation procedure, our hemorrhoid doctors use a handheld device that generates an intense beam of infrared light. A small probe is applied against the skin above hemorrhoid, exposing the tissue to a quick pulse of infrared light. The infrared light’s heat burns the tightly targeted area, coagulating the vein above hemorrhoid.
The resulting scar tissue cuts off the blood supply to the hemorrhoid, causing it to shrink and die. A scar forms on the wall of your anal canal where hemorrhoid has formed. As an added benefit, the scar tissue holds nearby veins in place so they don’t bulge into the anal canal and become hemorrhoids.
Is IRC Hemorrhoid Treatment Covered by Insurance? Is It Painful?
Most insurances usually cover infrared coagulation treatment, and you won’t need an overnight stay in a hospital. IRC is more effective than sclerotherapy, and you may tolerate it better than rubber band ligation in some cases.
What Does Infrared Coagulation Preparation Involve?
In most cases, no preparation is required. Our hemorrhoid doctor, the best gastroenterologist in NYC, will need to examine you in order to determine the best hemorrhoids treatment plan for your specific case.
What is Recovery like after IRC (infrared coagulation)?
It is normal to feel the need to urinate and experience minor rectal bleeding after each treatment. It is usually well-tolerated, but using a stool softener to help with bowel movements during healing can be helpful. Warm shallow baths, such as sitz baths, can also help in the healing process. Any concerning symptoms after your surgery should be discussed with your proctologist in NYC.
Laser treatment of hemorrhoids with IRC (infrared coagulation) is usually very well tolerated with minimal side effects.
What Are the Complications of Infrared Coagulation?
Although infection or bleeding can occur, infrared coagulation, the best hemorrhoid treatment in NYC, usually has few side effects or complications. Despite the fact that it is a relatively new technique, doctors have successfully used it to treat hemorrhoids across the country.
Our doctors recommend the following lifestyle changes to prevent the recurrence of hemorrhoidal disease. Increase the amount of fiber in your diet. Eating fiber-rich meals can soften the stools and make them easier to pass, ultimately helping treat and prevent hemorrhoids. Get some exercise, drink more water, and, if necessary, lose weight. A healthy diet, moderate exercise, and proper bowel habits will help you avoid this uncomfortable medical condition.
Hemorrhoid Banding
Hemorrhoid banding, also known as rubber band ligation, is a procedure in which a specialist uses a specialized instrument called a syringe ligator to wrap one or two tiny rubber bands around the base of an internal hemorrhoid. We use a banding kit accessory on the tip of a standard colonoscope for this procedure.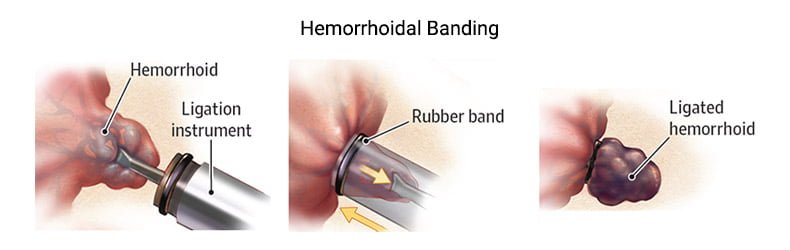
The rubber bands are wrapped around the hemorrhoidal column, reducing blood supply and causing piles to shrink. Treatment usually takes only a few minutes, but if you have multiple hemorrhoids, the procedure may take a little longer. Rubber band ligation is a common approach for removing medium-sized internal hemorrhoids.[4]
What is the recovery after hemorrhoid banding?
Treatment can be uncomfortable and cause bleeding at times, but the side effects are usually minor. To help prevent constipation, your doctor may recommend taking laxatives or using a stool softener. Once the piles have dried and withered, the bands usually pass with bowel movements. You should consult your doctor if you experience any troubling symptoms following your surgery
Surgical Options for Hemorrhoid Treatment. Do I need Surgery?
Only a small percentage of people require hemorrhoid surgery, and we will almost always prescribe it after other, less invasive procedures have failed. In certain cases, we recommend patients to a colorectal surgeon with whom we work closely. We can discuss the case with the surgeon in order to establish an effective treatment plan for your specific situation. You should discuss questions regarding further surgical options and recovery with your surgeon directly. We usually recommend surgery after less invasive procedures have been unsuccessful or are unlikely to be successful. Some of the surgical treatments that we may suggest are listed below.
Only a small percentage of people require hemorrhoid surgery, and we will most likely recommend it after other less invasive procedures have been unsuccessful.
What is Hemorrhoidectomy?
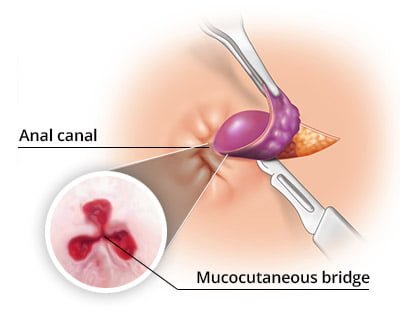
Hemorrhoidectomy is a type of surgery to remove internal or external hemorrhoids that are extensive or severe. Although it is associated with the most complications, surgical hemorrhoidectomy is the most effective treatment for hemorrhoidal disease. An excisional haemorrhoidectomy is a surgical technique to remove excess tissue that is causing the bleeding. The surgery can be performed under general anesthesia or using spinal anesthesia or sedation. It is a highly effective way to treat severe and recurring hemorrhoids, and the procedure cures 95% of cases. The risk of complications is low. During surgery, one or more incisions are made near hemorrhoid to remove it. The incisions are then closed or may be left open.
What Is Recovery After Hemorrhoidectomy Surgery?
You may be able to go home the same day as the surgery, or you may need to stay in the hospital for one night or longer. The incision may cause pain and bleeding for the first few days, and you may experience bleeding with bowel movements for several weeks after. Typically, 7 to 10 days off work are required.
What Is Stapled Hemorrhoidopexy?
Stapling hemorrhoids stop blood flow to the haemorrhoidal tissue and is typically used for prolapsed hemorrhoids.
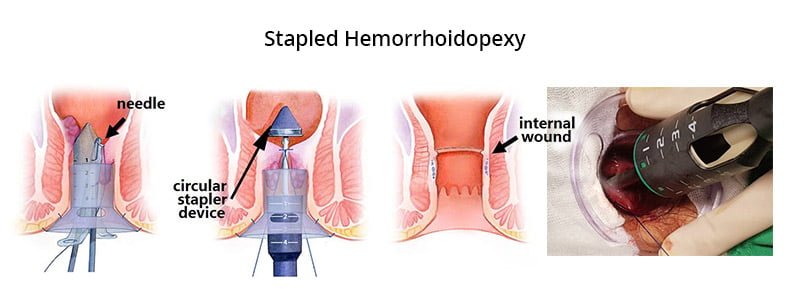
Your doctor will administer general anesthetic, local anesthesia, or spinal anesthesia before the procedure. You may feel some pressure during surgery if you choose local or spinal anesthesia, but you should not experience any pain. During surgery, the specialist uses specialized circular titanium staples to staple hemorrhoid’s base to the rectum wall. Fibrous tissue develops around the staples during healing, which helps to anchor hemorrhoids in place, restricting blood flow to them and decreasing swelling. Eventually, the staples pass out with bowel movements.
What is Recovery After a Stapled Hemorrhoidopexy?
After surgery, you may need to spend a night in hospital, and you may feel a sensation of pressure in your rectum for the first one or two days after. During the first few days, you may have a small amount of bleeding from your rectum. Bowel movements may cause some bleeding and discomfort for several weeks.
Frequently Asked Questions
How To Prevent Hemorrhoids?
One of the ways to prevent hemorrhoids is to keep your stool soft. If you’re wondering how to avoid hemorrhoids, we’ve put together a list of helpful tips:
- Drink a lot of water. To help keep your stool soft, we recommend drinking six to eight glasses of water a day.
- Eat high-fiber foods. Specialists recommend consuming more fruits, whole grains, and vegetables. These products soften the stool.
- Consider fiber supplements. The daily fiber intake should be around 20 and 30 grams. However, the majority of people do not consume the recommended amount. Numerous studies have shown that using fiber supplements over-the-counter improves the overall signs of hemorrhoidal disease.
- Exercise. Staying active can help prevent constipation and reduce pressure on your veins, which occurs when you stand for an extended period. Physical activity can also help you lose excess weight that may be causing your hemorrhoids.
- Do not sit for a long time. Sitting too long, especially on the toilet, can increase the pressure on the veins in the anus.
- Avoid straining. Holding your breath and straining when trying to pass a stool causes greater pressure in the veins in the lower rectum.
How Long Do Hemorrhoids Last?
It is impossible to give an exact time frame. Everything is dependent on how serious the problem is. If your hemorrhoids are small, your symptoms may go away in a few days without treatment. It may also be necessary to make minor changes to your diet and lifestyle. Prolapsed hemorrhoids that stick out of the anus might require treatment from a specialist and will take longer to heal.
Some women develop this condition during pregnancy because of the increased pressure in the abdomen. In this case, signs of this health condition will disappear after giving birth. Contacting a leading proctologist in NYC for an accurate hemorrhoid diagnosis and effective treatment is your best bet.
Are There Any Home Remedies for Hemorrhoids?
You can sometimes manage moderate pain, swelling, and inflammation of hemorrhoids with home treatments, such as:
- Aloe vera. Historically, people widely used aloe vera to treat hemorrhoidal disease and certain skin conditions. It is thought to have anti-inflammatory properties that assist in reducing irritation.
- Witch hazel. This product can help alleviate pain, itching, and swelling. It is available in liquid form and can be applied directly to hemorrhoids.
- A warm bath with Epsom salt. A warm bath can help relieve the irritation from hemorrhoids. We recommend taking a warm bath for 20 minutes after every bowel movement. You can achieve greater relief by adding Epsom salts to the bath.
Why Do Hemorrhoids Bleed?
Are Hemorrhoids Bad?
How Do Hemorrhoids Look and Feel?
Is It an Anal Fissure or a Hemorrhoid?
Are Hemorrhoids Contagious?
Can You Pop Hemorrhoid?
What About Diarrhea and Hemorrhoids?
How Can I Tell If It Is Hemorrhoids or Cancer?
Can Anal Sex Cause Hemorrhoids?
Can You Push a Hemorrhoid Back In?
Can Alcohol Cause Hemorrhoids?
What Are Alternative Names for Hemorrhoids?
Are There Any Specific Diets or Alternative Therapies for Hemorrhoids?
The most common piece of advice for the hemorrhoidal disease is to eat more fiber and stay hydrated. However, putting this advice into practice is not always so simple. Consider aiming for 25 to 30 g of fiber a day. This amount is more than twice what the average American consumes. Ideally, you should aim to drink six to eight glasses of water and other liquids each day, excluding diuretics such as alcohol and coffee. Lifestyle changes are used in many alternative hemorrhoid treatments. Listed below are a few tips to help alleviate the symptoms of this health issue. Consult your gastroenterologist about your treatment to ensure that it is the best next step for you.
- Avoid straining when trying to pass a stool, as this puts greater pressure on the veins in your lower rectum.
- If you feel the urge to pass a bowel movement, try to go as soon as you can.
- Exercise helps to prevent constipation.
Although these lifestyle changes can be beneficial, it is still necessary to consult a gastroenterologist for an accurate diagnosis and treatment plan. We look forward to meeting you.
As the best-in-class gastroenterologists, our hemorrhoid doctors provide highly personalized and comprehensive care. Their philosophies regarding the doctor/patient relationship are based on trust and have earned them some of the most respected reputations in New York.
For more information about hemorrhoid treatment options or to schedule a consultation with one of our hemorrhoid specialists, please contact our NYC gastroenterology office.


